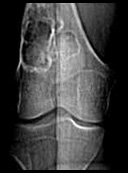
 History: A 19 year old woman with a five month history of right knee pain was radiographically found to have an 8.0 cm loculated well-defined, bubble-type lytic lesion with sclerotic borders involving the distal right femur in the meta-diaphyseal region (Fig. 1). The epiphysis was not involved.
History: A 19 year old woman with a five month history of right knee pain was radiographically found to have an 8.0 cm loculated well-defined, bubble-type lytic lesion with sclerotic borders involving the distal right femur in the meta-diaphyseal region (Fig. 1). The epiphysis was not involved.
The mass was curetted and yielded fragments of firm red-tan bone and soft tissue with a few small yellowish areas. Microscopically the tumor was hypercellular and composed of uniform spindled cells focally assuming a cartwheel or storiform whorled growth pattern (Figs. 2,3). There were scattered multinucleated osteoclast-like giant cells, foamy xanthoma cells and small amounts of collagen (Fig. 4). Some fields showed hemosiderin-laden stromal cells or macrophages. Neither mitoses nor significant pleomorphism were identified.
Diagnosis: “Non-ossifying Fibroma of Femurâ€
Mingyi Chen, MD, and Donald R. Chase, MD
Department of Pathology, Loma Linda University and Medical Center
California Tumor Tissue Registry
Discussion: Non-ossifying fibroma (NOF), also referred to as “non-osteogenic fibromaâ€, “fibrous cortical defect†or “metaphyseal cortical defect†was first described by Phemister in 1929. Sontag and Pyle later reported the radiological appearance in 1941, and in 1942 Jaffe with Lichtenstein described clinical, anatomical aspects and the natural history of the disease.
Non-ossifying fibroma is a common, non-neoplastic, self-healing lesion that occurs in skeletally immature individuals generally between the ages of 5 and 20 years. It is the most frequent skeletal lesion in children occurring in up to 30-40% and is generally found as an incidental radiographic finding. Although it is usually asymptomatic, larger lesions can cause chronic bone pain and possibly pathologic fracture if greater than half of the bone diameter is involved. The etiology of non-ossifying fibroma remains obscure. Since it consists of abundant fibrous tissue and may have hemosiderin deposition it has been suggested that it might be a reparative phenomenon to injury or be secondary to an abnormality at the epiphyseal plate.
NOF usually presents as a solitary lesion involving the metaphysis or meta-diaphyseal regions of long bones of the knee (distal femur, proximal tibia or fibula) or the distal tibia or proximal humerus. NOF on plain radiograph is eccentrically located, lytic, sharply demarcated, lucent and loculated lesion surrounded by a rim of sclerotic bone. The mass predominantly involves the lateral portion of the bone and produces mild cortical expansion. Biopsy is usually not warranted when the lesion occurs in the appropriate age group, in a typical site, and the x-rays are typical.
Multiple non-ossifying fibromas may be related to Jaffe-Campanacci syndrome which includes multiple extraskeletal congenital anomalies such as café-au-lait spots, mental retardation, hypogonadism or cryptorchidism, ocular abnormalities and cardiovascular malformations.
Differential Diagnosis:
• Fibrous Histiocytoma (FH) (“fibroxanthomaâ€) and NOF share identical histological features, the distinction being mostly based upon size and natural history. NOFs are asymptomatic, small (<3 cm) and well defined, eccentrically located, sclerotic bubble-type metaphyseal cortical defects which are self-limited and will usually regress. Conversely, fibroxanthomas are larger (>3 cm) intramedullary lesions that abut the cortex and typically scallop/erode the inner table of the cortex. They may occur in the pelvis, ribs or vertebrae and tend to occur in older patients. There are times, however, that distinction is impossible and it has been suggested that the two entities are related.
• Giant cell tumor (GCT) is characterized by occurrence in adults, an epiphyseal location and the absence of chondroid matrix. GCT tends to have less collagen than NOF and the giant cells are more evenly spaced. GCTs are also more likely to break through the cortex and involve soft tissue.
• Aneurysmal bone cyst (ABC) may also occur in young patients, and are characterized as expansile osteolytic lesions with thin walls containing blood-filled cystic cavities. Occasionally, ABC can extend to the subarticular cortex, mimicking a non-ossifying fibroma. Approximately 29% of ABCs are reported to be associated with some other solid bone lesion, 39% of which are giant cell tumors.
• Giant cell reparative granuloma (GCRP) is a benign reparative lesion that usually affects the small bones of the hands and feet or facial bones. It is histologically similar to giant cell tumors of bone.
• Chondromyxoid fibroma (CMF) may also occur in the metadiaphyseal region of the tibia and femur adjacent to the knee joint, and like NOF it radiographically may show large, expansile, bubbly lesions. Microscopically, in addition to fibrous elements and multi-nucleated giant cells, CMF contains varying amounts of chondroid and myxoid material.
In most cases a small non-ossifying fibroma requires no treatment because it is likely to resolve on its own. However if a pathological fracture occurs in a large lesion, curettage and bone grafting are likely to be required.
Suggested Reading:
Fechner RE, Mills SE. In: Atlas of Tumor Pathology: Tumors of the Bone and Joints. Fascicle 8, 3rd series. Washington, DC: Armed Forces Institute of Pathology. pp 145-50, 1993.
Fletcher C, Unni K, Mertens F. In: Pathology and Genetics of Tumours of Soft Tissue and Bone, IARC Press, Lyon, pp 31-35, 2002.
Campanacci M, Laus M, Boriani S: Multiple non-ossifying fibromata with extraskeletal anomalies: a new syndrome? J Bone J Surg; 65B:627-632, 1983.
Jaffe H, Liechtenstein L: Non-osteogenic fibroma of the bone. Am J Pathol 18:205-221, 1942.
Sontag L, Pyle S: The appearance and nature of cyst-like areas in the distal metaphyses of children. Am. J Roentgenol. 46:185-188, 1941.
Jaffe HL, Lichtenstein L. Non-osteogenic fibroma of bone. Am J Pathol, 18:205-21, 1942.