 History: A 20-year-old woman presented with chronic jaw pain and swelling in the left cheek. Computerized tomography (CT) scan identified an expansile, multilocular, osteolytic mass in the left lower maxillary sinus (Fig. 1). The mass had lobulated margins and contained microcystic elements with a large cyst measuring 24 mm. The mass was completely excised which showed dark red fluid inside the cysts. Grossly, the lesion contained heterogeneous, reddish-brown friable soft tissue fragments intermixed with hard components.
History: A 20-year-old woman presented with chronic jaw pain and swelling in the left cheek. Computerized tomography (CT) scan identified an expansile, multilocular, osteolytic mass in the left lower maxillary sinus (Fig. 1). The mass had lobulated margins and contained microcystic elements with a large cyst measuring 24 mm. The mass was completely excised which showed dark red fluid inside the cysts. Grossly, the lesion contained heterogeneous, reddish-brown friable soft tissue fragments intermixed with hard components.
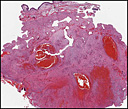
Histological sections demonstrated a moderately cellular spindle cell lesion with focal hemorrhage and cystic spaces. The cavities were filled with erythrocytes (Fig. 4) and bounded by fibrous tissue composed of spindle cells, numerous multinucleated giant cells, macrophages, and occasional xanthoma cells (foam cells). There was no true endothelial lining in the cystic walls. These histological findings were consistent with aneurysmal bone cyst (ABC). In addition, a marked reactive bone formation was present in the wall of the cysts. The intervened bony spicules contained irregular curvilinear/trabecular immature woven bones with a characteristic “C-shaped†or so called “Chinese characters” appearance (Fig. 2,3,5,6). The lacunae contained many viable osteocytes, but osteoblasts rimming in the osseous trabeculae was rarely present and helped establish a co-existent diagnosis of fibrous dysplasia (FD). The surgical procedure was carried out successfully and the patient had an uneventful recovery.
Diagnosis: “Aneurysmal bone cyst of the maxillary sinus associated with fibrous dysplasiaâ€
Mingyi Chen MD, Donald R. Chase MD
Department of Pathology, Loma Linda University and Medical Center
California Tumor Tissue Registry
(CTTR submission by Catherine Odell, M.D.)
Discussion: Aneurysmal bone cyst (ABC) is a benign, expansible cystic lesion of bone usually involving the metaphysis of long bones especially the femur, tibia, humerus, and posterior elements of vertebrae of patients younger than 20 years. The osteolytic lesion is often multilocular with blood filled spaces separated by fibrous septa containing fibroblasts, multinucleated osteoclast-type giant cells and reactive woven bone.
ABC arises de novo (primary ABC) in approximately 70% of the cases. Secondary ABC (about 30%) may complicate other benign or malignant bone lesions that have undergone hemorrhagic cystic change, including giant cell granulomas, osteoblastoma, chondroblastoma, fibromyxomas, angiomas, fibrous dysplasia (FD) and osteosarcoma.
About 2% of ABC is encountered in the head and neck regions with the jaws being the most frequently involved site. ABC of the jaw is usually associated with other bone pathology such as giant cell lesion or fibrous dysplasia (FD). In the maxillary sinus, ABC secondary to pre-existing fibrous dysplasia is found in the majority of the cases. Clinically, maxillary ABC presents as slowly progressive cheek swelling which may displace the soft palate and the eye. It may also cause nasal obstruction, recurrent sinusitis, dacryocystitis, and/or hypoaesthesia of the upper lip. It affects younger patients usually between 5 and 23 years of age.
The pathogenesis of ABC is unknown. Some authors believe that primary ABC results from resolution of a haematoma following local trauma. They speculate that ABC is usually a secondary phenomenon and histological evidence of previous bone pathology may be distorted or destroyed by the formation of the ABC. It is postulated that other pre-existing bone lesions may cause venous occlusion or an arteriovenous malformation and the consequent change in haemodynamics leading to ABC formation. Pre-existent fibro-osseous lesions such as FD have been shown in conjunction with ABC. It has also been speculated that increased vascularity in fibrous dysplasia (FD) may be a predisposing factor.
The diagnosis of ABC of the maxilla is usually suggested by radiographic imaging. It tends to be an osteolytic, eccentric, expansile mass with well defined margins with a so called “soap bubble†like or “blown out†appearance. CT and MRI studies usually show a multiloculated, heterogeneous contrast enhancing mass surrounded by a thin rim of bone and expansion of the maxillary sinus. There are usually distinct internal septa and characteristic fluid levels created by sedimentation of blood cells in the lesional cavities. In secondary ABC, CT and MRI may show evidence of an underlying primary lesion. If FD co-exists, plain X-rays generally show expansion of the maxillary sinus with calcified trabeculae giving a “ground-glass†appearance.
Microscopically, fibrous dysplasia consists of immature fibrillar or woven bony trabeculae surrounded by a relatively vascular and loose, hypocellular fibrous connective tissue stroma. The incompletely calcified bony trabeculae show some regularity in size and are uniformly distributed throughout, gradually blending into normal surrounding bone. Osteoclasts are inconspicuous, and osteoblastic rimming is present only when bone is being remodeled and occurs in stress lines.
The differential diagnosis of ABC associated with FD of maxillary sinus includes reparative giant cell granuloma, brown tumor of hyperparathyroidism and giant cell tumor.
• Reparative giant cell granuloma (central giant cell lesion/granuloma) is a localized benign but sometimes aggressive osteolytic proliferation consisting of fibrous tissue with hemorrhage and haemosiderin deposits, presence of osteoclast-like giant cells and reactive bone formation. ABC has more prominent cystic degeneration; typically clusters of giant cells surround cystic spaces. Actually, the solid variant of ABC shares may strikingly resemble a reparative giant cell granuloma.
• Brown tumor of hyperparathyroidism is morphologically indistinguishable from reparative giant cell granuloma. Determination of calcium and parathyroid hormone levels is most helpful.
• Giant cell tumor contains diffuse, evenly distributed, greater numbers of multinucleated giant cells showing no clustering. In ABC, the numbers of giant cells are much less but cluster in the cystic walls. In addition, ABC giant cells contain fewer nuclei than those of giant cells tumor. The mitotic figures (non-atypical forms) in ABC are fewer than is found in atypical forms of giant cell tumor. ABC exhibits prominent chronic inflammatory cells infiltrate in the background while giant cell tumor rarely has inflammatory changes.
In maxillary ABC, resection of the lesion is essential not only to establish the diagnosis but also to prevent further disease progression. Definitive diagnosis should be confirmed histologically as well as identification of any concurrent or pre-existing bone pathology. ABC is a benign condition but co-existing FD may undergo malignant degeneration in 0.5% of cases. Long follow-up of patients operated for ABC secondary to FD is recommended because disease may recur. Recurrent ABC can usually be managed effectively with further surgical resection.
Suggested Reading:
WHO Classification of Tumours Pathology and Genetics of Tumours of Soft Tissue and Bone. Edited by C.D.M. Fletcher, K. Unni, K. Mertens. pp338-339, 2002.
Differential Diagnosis in Surgical Pathology. Edited by Meryl H. Haber, Paolo Gattuso, Odile David, Daniel J. Spitz. pp722-723, 2001.
Fyrmpas G, Constantinidis J, Televantou D, Konstantinidis I, Daniilidis J.G. Primary aneurysmal bone cyst of the maxillary sinus in a child: case report and review of the literature. Eur Arch Otorhinolaryngol. 2006 Jul;263(7):695-8.
Hady MR, Ghanaam B, Hady MZ. Aneurysmal bone cyst of the maxillary sinus J Laryngol Otol. 1990 Jun;104(6):501-3.
Matt BH (1993) Aneurysmal bone cyst of the maxilla: case report and review of the literature. Int J Pediatr Otorhinolaryngol 25:217–226.
Kransdorf MJ, Sweet DE (1995) Aneurysmal bone cyst: concept, controversy, clinical presentation, and imaging. Am J Roentgenol 164:573–580.