 History: A 43-year-old gravida 0 woman with a history of menorrhagia was found to have a 3.5 cm left retroperitoneal, periaortic mass on abdominal CT six years previously (Fig. 1). She underwent CT-guided biopsy of the left periarotic mass and was diagnosed to have an epithelioid and spindle cell neoplasm consistent with epithelioid leiomyosarcoma. Despite chemotherapy the retroperitoneal lesion persisted, though no progression was seen by CT follow-up. A current pelvic examination demonstrated a mobile anteverted enlarged uterus without adnexal masses. A vaginal hysterectomy with bilateral salpingo-oophorectomy was performed.
History: A 43-year-old gravida 0 woman with a history of menorrhagia was found to have a 3.5 cm left retroperitoneal, periaortic mass on abdominal CT six years previously (Fig. 1). She underwent CT-guided biopsy of the left periarotic mass and was diagnosed to have an epithelioid and spindle cell neoplasm consistent with epithelioid leiomyosarcoma. Despite chemotherapy the retroperitoneal lesion persisted, though no progression was seen by CT follow-up. A current pelvic examination demonstrated a mobile anteverted enlarged uterus without adnexal masses. A vaginal hysterectomy with bilateral salpingo-oophorectomy was performed.
The 920 gm, 19.0 x 18.0 x 8.0 cm uterus contained multiple serosal, intramural and submucosal nodules with pale-tan whorled cut surfaces measuring up to 8.0 cm in diameter (Fig. 2a). Additionally, the anterior lower uterine segment was distorted by numerous firm, poorly-circumscribed nodules ranging from 0.2 to 1.0 cm in diameter. The excised 6.0 cm left periaortic mass proved to be an enlarged lymph node with fleshy-pink, homogeneous cut surfaces (Fig. 2b).
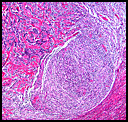
Microscopically, the lower uterine segment was extensively infiltrated by numerous small nodules with irregular tongues invading the adjacent myometrium (Fig. 3). The nodules were densely cellular with a “blue” appearance at low magnification and areas with prominent stromal hyalinization (Fig. 4). Composed of a spindle cell proliferation, the neoplasm was punctuated by a plexiform capillary network with edematous change (Fig. 5). Spindle cells featured uniform oval to round nuclei, vesicular chromatin, small nucleoli and elongated inconspicuous cytoplasm (Fig. 6). No striking pleomorphism and relatively few mitotic figures were seen ranging from 2 to 5 mitoses per 10 hpf with occasional atypical forms. No hemorrhagic necrosis, definitive vascular invasion, sex cord-like arrangements, or epithelioid differentiation was identified. The periaortic lymph node was predominately replaced by neoplastic cells with identical histology as the lower uterine segment nodules (Fig. 7). Immunohistochemical studies performed on both the uterine and lymph node tumors exhibited identical patterns: strong positivity for CD10, focally positivity for SMA, and negative staining for desmin (Fig. 8a & 8b). A Ki67 proliferative index demonstrated low activity (~ 10%).
Diagnosis: “Low-grade endometrial stromal sarcoma with retroperitoneal periarotic lymph nodes metastasisâ€
Mingyi Chen M.D., Evelyn Choo M.D., Amita T. Mistry, M.D., Donald R. Chase, M.D.
Department of Pathology, Loma Linda University and Medical Center
California Tumor Tissue Registry, Loma Linda, California
Discussion: Endometrial stromal tumors are the second most common category of mesenchymal tumors of the uterus; however, they only account for approximately 10% of all uterine sarcomas. Low-grade endometrial stromal sarcoma (LGESS) occurs in younger women (median age ~40 years) compared to other uterine neoplasms such as carcinosarcoma (malignant mullerian mixed tumor), leiomyosarcoma, or endometrial carcinoma. Patients typically present with abnormal vaginal bleeding, pelvic pain, and a clinical impression of uterine leiomyomata due to an enlarged uterus with an irregular contour.
Endometrial stromal tumors are divided into two classes based on the presence of circumscribed margins (stromal nodule), or infiltrating margins with or without vascular intrusion (stromal sarcoma). The two lesions are otherwise indistinguishable histologically. Infiltration is seen as irregular, jagged islands or tongues of neoplastic stromal cells between the smooth muscle bundles of the surrounding normal myometrium.  Determining myometrial infiltration can be problematic, especially when there is subtle interdigitation of stromal and smooth muscle cells at a compressive margin examined at high magnification, which should not be counted as an infiltrative margin. A diagnosis of stromal sarcoma is rarely possible in curettage and biopsy specimens since margin evaluation is questionable. For vascular involvement, clumps of tumor cells must be present in spaces within the myometrium.
LGESS is comprised of uniform, oval to spindle-shaped cells with inconspicuous cytoplasm and round to oblong nuclei that are morphologically, ultrastructurally and immunohistochemically identical to endometrial stromal cells found in proliferative endometria. This monotonous cellular proliferation is interrupted by a characteristic regular network of delicate ramifying small vessels resembling spiral arteries and capillaries. The presence of fragments of proliferative phase endometrial stroma without glands in curettage or biopsy specimens raises the possibility of an endometrial stromal tumor. Significant cytological atypia and pleomorphism are absent as well as stainable glycogen and mucin. Occasionally, an abundance of distinctive hyalinized osteoid-like collagen is present, and may be so extensive as to reduce the cellular component to attenuated chains of cells, resembling a hyalinized leiomyoma. This pattern of hyalinization may be preserved in pelvic recurrences and pulmonary metastases. Foam cells may be present in stromal neoplasms and are morphologically identical to the foam cells seen in endometrial hyperplasia and carcinoma. Neoplastic cells are positive for CD10, almost always estrogen and progesterone receptor positive and focally positive for actin.
The most common cytogenetic alteration observed in low-grade endometrial stromal tumors is the t(7;17)(p15;q21) translocation, resulting in the fusion of the JAZF1 and JJAZ1 genes.
Differential Diagnosis:
•   Benign smooth muscle tumors: In a uterine tumor composed of uniform spindle cells with circumscribed margins, the distinction between smooth muscle and endometrial stromal tumors is less critical since both leiomyoma and endometrial stromal nodules are benign. With infiltrating margins, the distinction between either a leiomyoma or a LGESS is clinically significant. Cellular leiomyomata can be especially problematic. As in the current case, the concomitant presence of extensive leiomyomas can cause difficulties in the diagnosis of endometrial stromal sarcoma. Small tissue sampling can also add to the complexity. Positive staining of desmin, smooth muscle actin, and/or CD10 immunostains can be helpful in distinguishing LGESS from smooth muscle neoplasms. If the cellular lineage remains ambiguous, it may be prudent to assign the tumor to the low-grade stromal category, particularly if there are tongue-like islands infiltrating within the myometrium or vascular invasion is present. Though unequivocal smooth muscle elements may be seen within otherwise typical endometrial stromal neoplasms, such tumors behave more like LGESS than their smooth muscle counterparts (such as intravascular leiomyomatosis, leiomyomatosis, or leiomyomas). Intravascular leiomyomatosis is far less common than endometrial stromal sarcoma; and should not be diagnosed unless tumor cells show unambiguous smooth muscle differentiation.
•   Leiomyosarcoma: LGESS lacks significant cytological atypia and is less mitotically active when compared to leiomyosarcoma. Mitotic indices more than 10 mitotic figures/10 hpf are unusual in endometrial stromal sarcoma but do not exclude the diagnosis. In addition, the tumor cells in leiomyosarcoma have more abundant cytoplasm, and can often be focally arranged in long fascicles. Angioinvasive leiomyosarcoma is distinguished from endometrial stromal sarcoma by its greater cytologic atypia, and lack of plexiform vasculature.
•   Adenomyosis: Occasionally, adenomyotic foci do not contain glands, raising the possibility of LGESS. Stromal nodules and sarcomas produce mass lesions, whereas small foci of gland-free endometrial stroma in the absence of a mass within the myometrium are almost always a manifestation of adenomyosis. Looking for the characteristic smooth muscle hypertrophy that often accompanies adenomyosis as well as gland-containing lesions elsewhere in the myometrium usually establishes the correct diagnosis. Very rarely, fragments of benign proliferative phase stroma without glands are found within myometrial vessels. As long as no mass lesion is identified and the intravascular fragments are microscopic, this phenomenon is undoubtedly a manifestation of adenomyosis.
•   Hemangiopericytoma: Vasculature resembling endometrial spiral arterioles is uniformly distributed throughout LGESS potentially leading to a mistaken diagnosis of hemangiopericytoma. Immunohistochemical studies can establish the diagnosis with CD10 staining the endometrial stromal cells in LGESS, and the weak and patchy staining of CD34 in hemangiopericytoma.
•   Adenosarcoma and malignant mullerian mixed tumor (MMMT): LGESS with foci of glandular differentiation raises the differential diagnostic consideration of adenosarcoma which contains endometrial stromal cells as the mesenchymal component. Glands in endometrial stromal sarcoma are usually sparse and small without surrounding stromal condensation, whereas those of adenosarcoma often feature periglandular stromal condensation and tend to be large and dilated. However, when glands are numerous and stromal condensation is questionable, considerable overlap exists between these two neoplasms with malignant mesenchymal elements. LGESS typically expresses estrogen and progesterone receptors, but MMMT shows marked pleomorphism and a high mitotic rate. Prognostically, both LGESS with glands and adenosarcoma with a low-grade stromal proliferation are low-grade neoplasms, though the prognosis worsens when the primaries occur in extra-uterine sites.
LGESS is characterized by indolent growth with up to half of all patients developing one or more pelvic or abdominal recurrences, some as much as 20 years later. Median interval for recurrence is 3-5 years. Women with stage I disease have >80% survival, while survival is less favorable (~50%) when advanced stage disease is present. Pulmonary metastases occur in 10% of stage I tumors. The single most important prognostic factor is the stage at presentation, and risk of recurrence is determined by both stage and the type of surgical procedure. Adnexal spread may not be appreciated during the operation and pelvic recurrence occurs more frequently with ovary conservation. Both recurrent and metastatic disease can remain localized for long periods and are amenable to successful treatment by resection, radiation therapy, progestin therapy or a combination thereof. Curative therapy is not guaranteed by bland histology and low mitotic indices. Although progestin therapy may be effective in cases with progesterone receptor expression, chemotherapy alone is usually ineffective.
Suggested Reading:
1.   Kempson RL, Hendrickson MR. Smooth muscle, endometrial stromal, and mixed Mullerian tumors of the uterus. Modern Pathology. 13(3):328-42, 2000.
2.   Clement PB, Young, RH. Atlas of gynecologic surgical pathology. 1st Edition, 177-210, 2000.
3.   Kurman RJ. Blaustein’s pathology of female genital tract. 5th Edition, 583-605, 2002.
4.   Robboy SJ, Anderson MC, Russell P. Pathology of the female reproductive tract. 1st Edition, 370-80, 2002.
5.   Kurihara S, Oda Y, Ohishi Y, Iwasa A, Takahira T, Kaneki E, Kobayashi H, Wake N, Tsuneyoshi M. Endometrial stromal sarcomas and related high-grade sarcomas: immunohistochemical and molecular genetic study of 31 cases. Am J Surg Pathol. 32(8):1228-38, 2008.